Everything You Need to Know About Blood Vessel Removal
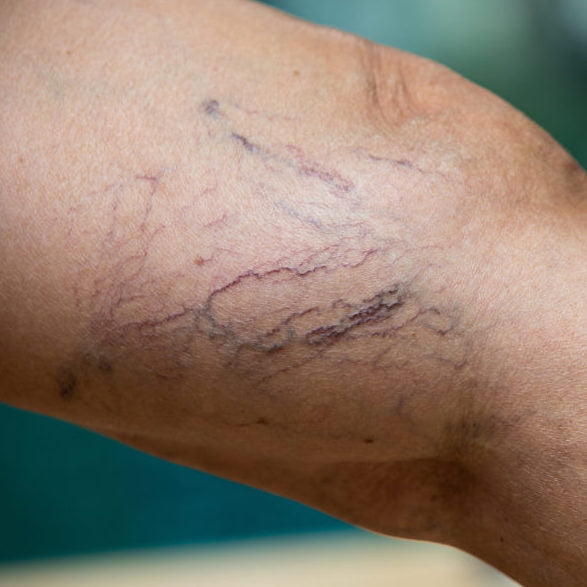
Have you noticed little red lines creeping and crawling across your skin? This bothersome network can be attributed to broken blood vessels — also known as telangiectasia, broken capillaries, and spider veins. Once they make an appearance, these tricky, thread-like nuisances don’t always go away on their own. In fact, they can actually increase in…
Published:
4 minute read
Have you noticed little red lines creeping and crawling across your skin? This bothersome network can be attributed to broken blood vessels — also known as telangiectasia, broken capillaries, and spider veins. Once they make an appearance, these tricky, thread-like nuisances don’t always go away on their own. In fact, they can actually increase in number over time, causing your skin to take on a ruddy, blotchy appearance.
Luckily, dermatologists can zap these broken blood vessels into oblivion. Here, we explore what causes blood vessels to “break” and the treatments that help stop this unsightly network from growing.
What causes broken blood vessels?
Technically, these blood vessels don’t “break.” Prolonged UV exposure, genetics, and the natural aging process — cause the walls of your healthy blood vessels to atrophy (that’s the scientific word for stop working) and dilate.
Dilation is a sudden widening and constricting that makes your blood vessels become visible under the skin. But it doesn’t stop there. Increased estrogen hormones during pregnancy, the skin condition rosacea, injuries that cause bruising, excessive heat through weather changes or exercise, and exposure to chemical irritants can also dilate blood vessels. We hate to be Debbie downers, but on top of that, alcohol consumption, even when moderate, can contribute to broken blood vessels, and severe binge drinking can worsen the condition. Even vomiting or violently sneezing can create intense pressure in your face, causing blood vessels to dilate and break! Because there’s a laundry list of potential causes for a capillary to “burst,” we advise that you visit your dermatologist to determine the underlying condition and can figure out your best mode of treatment.
I’m definitely seeing a web of red forming on my face. How can I get rid of it?
The good news: Various in-office treatment options exist for blood vessel removal, and are often used in tandem to best address your needs. Vascular laser therapy is a preferred treatment plan for blood vessels, but there are different lasers to choose from. The VBeam, a pulsed dye laser, emits a 595-nanometer wavelength of light energy that passes through the epidermis and some of the dermis (up to 1.2 mm deep) and works like a heat-seeking missile. More specifically, the hemoglobin that’s found in red blood cells absorbs the wavelength of this laser, while other nearby structures don’t. This allows it to pinpoint its target effectively, without disturbing the surrounding tissues. This light energy is converted to heat energy, which then “destroys” the offending blood vessels and its surrounding vessel walls. Depending on the VBeam pulse duration your dermatologist recommends, you can either “one-and-done” your removal by rupturing the blood vessel quickly in one visit (with bruising for five to seven days), or you can use the non-purpuric lower heat setting which is less immediately effective and requires several treatments (but no bruising).
Another common laser is the KTP laser, which is a solid-state laser and has a wavelength of 532 nanometers. It’s effective at treating vascular lesions (such as spider veins and telangiectasias) in a purpura-free manner — which is doctor speak for without causing bruising. It’s also popular for removal of lentigines (sun spots) and other small pigmented lesions.
Other, newer sophisticated solid-state lasers, such as the Excel V, offer two wavelengths (532 nanometers and 1064 nanometers) of light — it’s a combination of the KTP laser we mentioned above and the Nd:Yag laser — and it can target a wide range of vascular lesions, including larger blood vessels that appear as red webs and bluish vein-like threads. Typically, only one to two sessions are needed to achieve desired results. Downtime is nil, with skin left pinkish for a few hours where treated.
Aside from lasers, Intense Pulsed Light (IPL), which delivers various wavelengths (between 500 and 1200 nanometers) in each pulse of light instead of just one wavelength like a laser, can be used for blood vessel removal as well. However, because their energy output is scattered, they aren’t as effective at hitting one target (like blood vessels), yet they could be a good option for patients who are looking to tone down redness, hit hyperpigmentation and zero in on sun damage all at once. These are ideal for people struggling with rosacea or conditions like poikiloderma of Civatte. You might need three to six treatments spaced a month apart, depending on the severity of the broken capillaries.
And if you’re worried about pain, “snap” out of it: Both IPL and laser treatments tend to feel like a rubber band snapping against your skin. Since sessions are fairly quick (as little as 5 to 20 minutes), it’s only a small amount of discomfort.
So, do my broken blood vessels disappear right after treatment?
Unfortunately, lasers and IPL aren’t magic. They will cause blood vessels to fade, but it may take several weeks or even months for them to disappear. This will be contingent on the type of treatment and amount of treatments you’ve gotten. And just know that, depending on the underlying cause, more broken capillaries could form in their place.
Is everyone a candidate for blood vessel removal?
If you take certain acne medications, you’ll be asked to put these on hold leading up to the treatment. Sadly, darker complexions don’t fare well with some lasers; the heat used to zap blood vessels can actually cause pigmentation, darkening the area. However, it’s always smart to talk with your dermatologist about your available options and what best meets your needs. With so many choices available, there’s definitely a safe and effective way to target your broken blood vessels.
Dr. Betty Yan, a dermatology resident at Southern Illinois University School of Medicine (SIU), helped contribute to the accuracy of this story.








