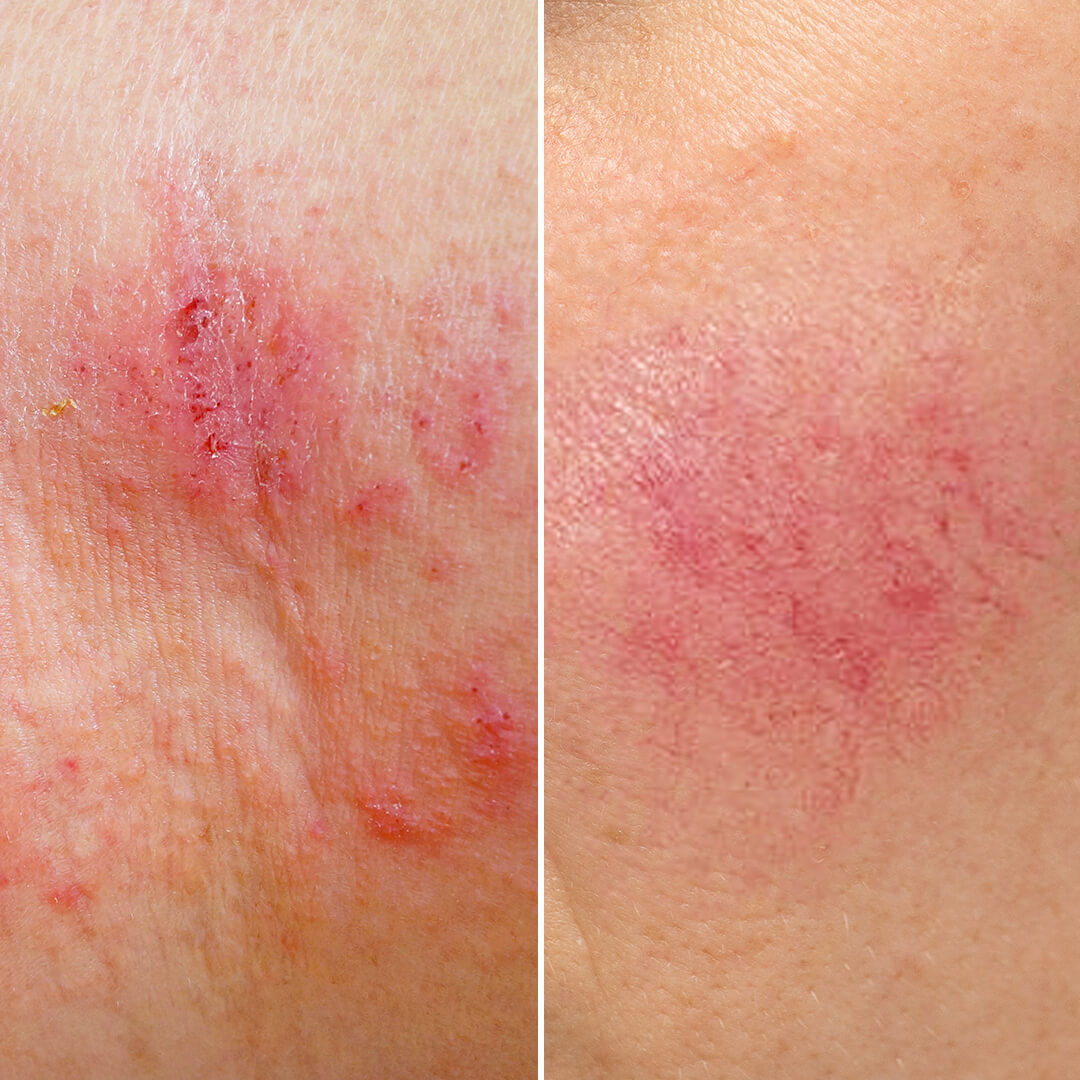
Eczema vs. Rosacea: Key Differences, Symptoms, and Treatments
Red, irritated skin could be a sign of one of these conditions, says Dr. Pimple Popper. Here's her advice.
Published:
3 minute read
If you've ever dealt with red, irritated skin that seems to flare up out of nowhere, you're not alone. Two of the most common chronic skin conditions in the U.S. are eczema and rosacea. While they might look similar at first glance, these conditions have their own unique triggers and treatments. Understanding what sets them apart can help you manage your symptoms more effectively.
So how do you tell the difference between eczema and rosacea? We turned to board-certified dermatologist Dr. Sandra Lee (aka Dr. Pimple Popper) for answers.
Article Quick Links

What is eczema? An overview
Sometimes called atopic dermatitis, eczema affects over 30 million Americans of all ages and ethnicities. We’ve covered the condition in detail here. Eczema typically presents as a dry, red, itchy rash that may be scaly or bumpy. Commonly affected areas include the elbows, knees, hands, feet, upper chest, neck, and face.
- Symptoms: Dry, red, itchy, scaly, or bumpy rash; fluid-filled blisters; scabbing from scratching.
- Causes: Genetic variation affecting skin barrier function, potential mutation in the filaggrin gene.
- Treatments: Lifestyle changes, moisturizing skincare, OTC hydrocortisone, prescription steroids, and biologics.

What is rosacea? An overview
Rosacea affects over 16 million Americans, primarily adults over 30. It often manifests as redness or flushing on the face, with possible papules and pustules resembling acne. Rosacea can also cause skin thickening, particularly on the nose (rhinophyma), and visible blood vessels (telangiectasia). For a more in-depth look, check out our rosacea blog.
- Symptoms: Redness, flushing, papules, pustules, skin thickening, visible blood vessels, dry/red eyes.
- Causes: Genetics, innate immune system irregularities, neurovascular issues, microbial imbalances.
- Treatments: Avoiding triggers, gentle skincare, sunscreen, light/laser therapy, topical retinoids, oral antibiotics.
How to tell the difference between eczema and rosacea
A dermatologist is the best person to determine the cause of your red, inflamed skin, notes Dr. Lee — but here's a guide that may help.

Dr. Pimple Popper's Gentle Skincare Picks
Dr. Pimple Popper’s skincare tips for eczema and rosacea
Because every patient is unique, it’s important to consult with your dermatologist if you suspect you have a chronic skin condition like eczema or rosacea. Dr. Lee always suggests a tiered approach for managing any skin concerns: start with over-the-counter solutions, then move to stronger treatments — including prescription options — if necessary.
- Bathe/cleanse with warm water (not hot): Hot water can trigger rosacea flares and dehydrate eczema-prone skin.
- Avoid harsh physical scrubs: Things like nut shells, sugar, and coffee grounds can cause micro tears, worsening both conditions.
- Use alpha hydroxy acids carefully: Start slow and watch for sensitivity. Glycolic acid can help but should be used under guidance.
- Support the skin’s natural barrier function: Keep skin hydrated and moisturized with nourishing ingredients like hyaluronic acid.
- Calm inflammation from eczema with OTC hydrocortisone cream: Typically used for up to 7 days (not recommended for rosacea treatment).
Dr. Pimple Popper answers your eczema and rosacea FAQs
- Q: Can stress cause both eczema and rosacea?
- A: Yes, stress is a common trigger for both conditions. Managing stress (through practices like exercise and meditation) can help with this.
- Q: Are the treatments for eczema and rosacea the same?
- A: While some treatments overlap, such as avoiding triggers and using gentle skincare, specific medications and therapies differ. Visit our eczema and rosacea blogs for detailed information.
- Q: Can I use the same skincare products for both conditions?
- A: Some products are suitable for both, but it’s crucial to choose ones that support the skin barrier and are free of irritants. Consult your dermatologist for personalized advice.

Dr. Lee's Last Word
Eczema and rosacea are two of the most common inflammatory skin conditions that I treat in my practice. Though not life-threatening, these disorders can be disruptive and impact a patient’s self-esteem. Maintaining a healthy skin barrier and avoiding triggers can go a long way toward managing symptoms.

























