Our Guide to Managing Psoriasis
More than 8 million Americans suffer from psoriasis, a chronic inflammatory disorder that results in plaque formation on the surface of the skin. If you’ve ever noticed scaly, inflamed patches of skin on your body, you might be one of them. While these flare-ups can be scary and annoying, proper treatment can dramatically clear them up. We consulted our founder and board-certified dermatologist, Dr. Sandra Lee, for the best plan of action to diagnose and treat psoriasis.
Published:
2 minute read
More than 8 million Americans suffer from psoriasis, a chronic inflammatory disorder that results in plaque formation on the surface of the skin. If you’ve ever noticed scaly, inflamed patches of skin on your body, you might be one of them. While these flare-ups can be scary and annoying, proper treatment can dramatically clear them up. We consulted our founder and board-certified dermatologist, Dr. Sandra Lee, for the best plan of action to diagnose and treat psoriasis.
What Is Psoriasis?
While the exact cause of this disorder is unknown, it’s likely the result of problems with the body’s autoimmune system. Psoriasis typically affects the skin on the scalp, joints, hands, and lower body, including the knees, elbows, lower back, feet and genitals.
Adults and children can be diagnosed with psoriasis, but the disorder commonly presents when people are in their 20s. The thick patches of skin associated with psoriasis fluctuate depending on stress levels, environmental conditions and the presence of infection.
Most people who have psoriasis initially assume they have a skin infection or are experiencing an allergic reaction. Once they see a doctor, however, diagnosing psoriasis is relatively easy, but in some cases a skin biopsy is required.

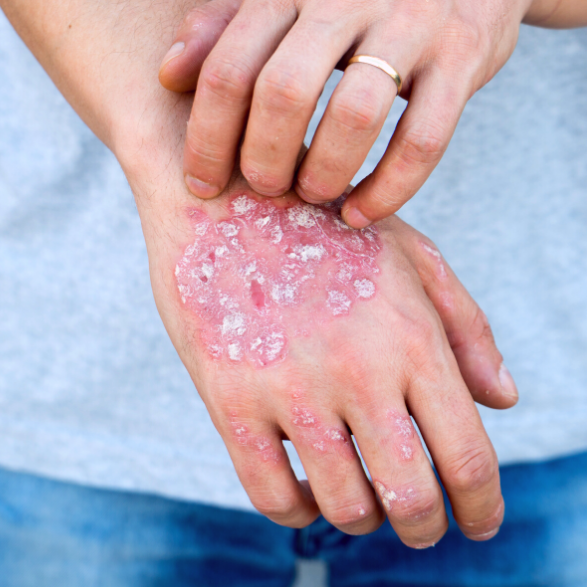
What does psoriasis look like?
This skin disease is characterized by raised, red and silvery irritated patches of dead skin cells that appear on the body’s surface. Psoriasis causes your skin cells to divide too quickly, multiplying up to 10 times faster than normal cells, and prevents your body from shedding them. This leads to a build-up of skin cells, forming thick, irritating patches that are almost always painful and itchy, and may bleed and crack.

How do you treat psoriasis?
Once psoriasis has been diagnosed, it’s time to look into treatment options. The type of treatment a doctor will advise will depend on how much of the skin’s surface is affected, the thickness of the plaques, and if the individual is also suffering from arthritis.
At any stage of the treatment process, you should be using a moisturizer consistently. Look for one that’s rich in emollients to combat dryness, itching and flaking.
Hydrocortisone cream is often considered the first line of defense against the persistent itch associated with psoriasis. Medical hydrocortisone is a synthetic version of the hormone your body naturally creates to fight inflammation. Hydrocortisone cream can be highly effective in alleviating the more disruptive symptoms of psoriasis and can even reduce the size of the lesion considerably.
Can you prevent psoriasis?
Like many skin conditions, lifestyle choices can both trigger and alleviate psoriasis. Dr. Lee recommends eating an anti-inflammatory diet — heavy in fruits, vegetables, probiotics and Vitamin D. Try to limit your alcohol consumption and smoking as they can exacerbate psoriasis flare ups.
You’ve probably learned not to pick at your breakouts, but it’s time to apply that to your psoriasis patches. Picking at scaly skin can severely worsen the spots, so stick to your treatment regimen and keep your hands off!
Although psoriasis is common, flare-ups can still be debilitating. As frustrating as a chronic condition is, sticking to the treatment plan prescribed by your doctor and incorporating an emollient moisturizer and hydrocortisone cream can make a huge difference!





