Do You Have Skin-Picking Disorder? Signs and Treatments for Dermatillomania
Dr. Pimple Popper) explains when picking becomes a problem — and what to do about it.Published:
5 minute read
We all pick at our skin: whether it’s squeezing blackheads, peeling cuticles, or scratching at a scab — it’s human nature. While the habit can be satisfying in the moment, we’re often left wishing we’d just left it alone.
According to board-certified dermatologist Dr. Sandra Lee (aka Dr. Pimple Popper), occasional skin picking (though ill-advised) isn’t necessarily a problem — but it can turn into one. We wondered: when is it OK to pick at your skin, and when is it an issue? In other words, how can you tell the difference between overzealous grooming, and whether you have clinical skin-picking disorder?
Article Quick Links
What is skin-picking disorder (excoriation disorder)?
Clinical skin picking — also known as excoriation disorder or dermatillomania — is a mental illness classified as a Body-Focused Repetitive Behavior (BFRB) in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). More common in females, it tends to develop during puberty and is estimated to affect between 2-3% of American adults.
Excoriation disorder is closely related to obsessive-compulsive disorder (OCD). People with this condition cannot control their compulsive picking, which is often triggered by anxiety and emotional stress. There are two main types of skin picking:
- Focused: The person is aware of and concentrating on the picking.
- Automatic: The person is preoccupied with something else (like watching TV) and picking unconsciously.
What causes skin-picking disorder?
Scientists aren’t entirely sure what leads some people to develop dermatillomania. It’s more common in those who have family members with the disorder, which suggests a genetic component. In addition, excoriation disorder is commonly associated with other mental illnesses, including:
- Depression
- Anxiety
- Obsessive-compulsive disorder (OCD)
- Nail-biting
- Trichotillomania (aka hair-pulling disorder)
Signs you might have skin-picking disorder
Chances are, you’ve been unable to resist trying to pop a pimple (or an ingrown hair?) that just wasn’t ready — and ended up with an angry red welt. Or you can remember as a kid, scratching away at a scab until it started bleeding again. Does this mean you have skin-picking disorder? Probably not.
Here are some common signs that could indicate a more serious problem:
- Spending excessive time picking at skin imperfections, both real and perceived.
- Picking, scratching, or squeezing to the point of causing noticeable damage.
- Feeling unable to stop picking, even when it leads to infections, scarring, or emotional distress.
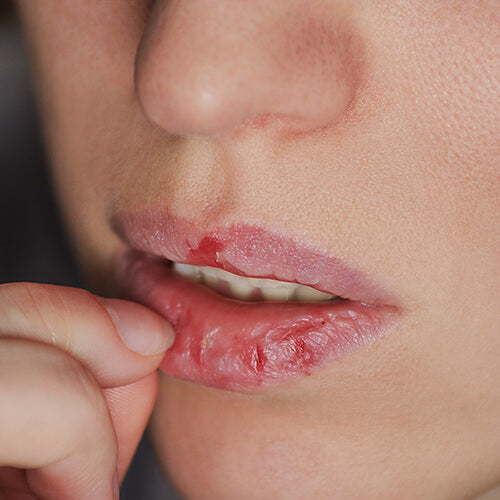
- Focusing on specific areas like the face, scalp, arms, or fingernails.
If these behaviors sound familiar, consulting a dermatologist or mental health professional can help determine whether excoriation disorder might be the cause.
How is skin-picking disorder diagnosed?
Excoriation disorder is classified as a mental health condition in the DSM-5, which provides specific criteria for its diagnosis. Clinicians look for behaviors and patterns such as:
- A fixation on real or perceived skin imperfections, leading to compulsive behaviors.
- Skin picking, scratching, squeezing, or rubbing that results in visible lesions, scarring, or tissue damage.
- Recurrent infections or frequent use of bandages, makeup, or clothing to conceal skin damage.
- Persistent attempts to stop the behavior, with repeated relapses despite intervention.
- Significant disruption to daily life, including avoidance of social activities or work.
- Emotional distress or social isolation caused by the behavior.
It’s also important to rule out other potential causes, such as self-harm behaviors, dermatological conditions like eczema, or side effects of medications. A thorough evaluation by a mental health professional or dermatologist is key to developing an effective treatment plan.
Treatment for skin-picking disorder
Managing excoriation disorder often requires a combination of approaches to address both the physical and emotional impacts. Treatment options include:
- Cognitive-behavioral therapy (CBT): This type of talk therapy helps individuals identify triggers, manage compulsive behaviors, and replace them with healthier habits.
- Medications: Selective serotonin reuptake inhibitors (SSRIs) and other medications prescribed by a mental health professional can help reduce compulsive urges.
- Self-help strategies: Keeping your hands occupied with fidget toys, stress balls, or wearable barriers like gloves can reduce picking behaviors.
- Dermatological treatments: A dermatologist can recommend topical treatments to heal damaged skin and minimize scarring.
If you’re struggling with excoriation disorder, seeking help from a mental health professional or dermatologist can make a significant difference.
Dr. Pimple Popper's "Stop the Pop" Treatments
How to stop picking at your skin
Maybe you don’t have dermatillomania — but you do sometimes feel like you just can’t keep your hands away from a tempting pimple, or that peeling sunburn. To prevent unnecessary inflammation or even scarring, it’s best to just let your skin do its thing. To encourage healing, Dr. Lee says not to pick, squeeze, or pop your pimples. It usually makes them worse and can even cause scarring.
To keep your skin healthy and support healing, Dr. Lee recommends these tips:
- Use acne patches: These clear, protective patches not only speed up healing but also reduce the urge to pick. Try SLMD Salicylic Acid Pimple Patches.
- Apply spot treatments: Target pimples with products containing salicylic acid or benzoyl peroxide to reduce inflammation and encourage healing.
- Keep your hands busy: Fidget toys, stress balls, or other distractions can help break the habit of picking.
- Cover healing areas: Use bandages or lightweight clothing to protect vulnerable spots while they heal.
- Moisturize regularly: Dry or peeling skin can make you want to pick. Keep your skin hydrated with a non-comedogenic moisturizer to reduce temptation. Try SLMD Hyaluronic Acid Moisturizer, Facial Moisturizer with Vitamin C.
Dr. Pimple Popper answers skin-picking disorder FAQs
Q: Is skin-picking disorder curable?
A: While there isn’t a cure, excoriation disorder can be effectively managed with therapy, medications, and self-help strategies. Consistent treatment can significantly reduce symptoms and improve quality of life.
Q: What should I do if I feel the urge to pick my skin?
A: Try keeping your hands busy with fidget toys or stress balls. Cover affected areas with bandages or hydrocolloid patches to protect healing skin and reduce the temptation to pick.
Q: Can a dermatologist help with skin-picking disorder?
A: Yes, a dermatologist can treat the physical effects of skin picking, such as scarring or infections, and collaborate with mental health professionals for a comprehensive approach.

Dr. Lee's Last Word
I’m a realist: I know people are going to pop their pimples, or pick at their peeling skin. As a dermatologist, I have to say that this can definitely lead to problems — but usually, it’s not too harmful. Excoriation disorder, however, is a serious mental health issue that affects not just a person’s skin health, but their overall well-being. Please reach out to a doctor if you, or someone you know, is struggling.