Dr. Pimple Popper’s Perspective: Keratosis Pilaris
Your favorite dermatologist weighs in on what causes "strawberry skin" — and what you can do about it.
Published:
3 minute read
Keratosis pilaris — sometimes called “chicken skin” or "strawberry skin" — is one of the most common concerns that dermatologists hear about from patients.
Fortunately, it’s one of the easiest to manage, with the right skincare. To learn more about what causes keratosis pilaris, and the best way to treat it, we talked to dermatologist and SLMD Skincare founder, Dr. Sandra Lee, aka Dr. Pimple Popper.
Article Quick Links
What is keratosis pilaris?
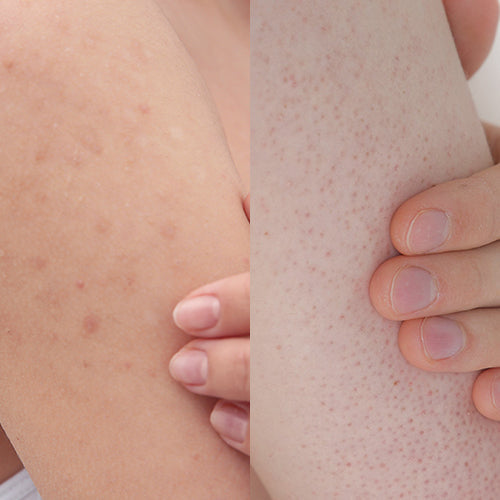
DPP: This is one of the skin concerns patients talk to me about most frequently. Keratosis pilaris is a condition that causes tiny, rough bumps on the backs of your arms, on your thighs and buttocks — sometimes on your cheeks as well. It tends to start in childhood, and some patients grow out of it eventually.
KP is often associated with dry skin, and it can sometimes be itchy but it’s usually not too uncomfortable. Some patients experience redness along with the bumps, and that’s known as keratosis pilaris rubra. It’s one of those conditions that’s typically cosmetic, but if you pick or scratch at it, there is a chance you could create irritation.
What causes keratosis pilaris?
DPP: The word keratosis means “scaly skin” and pilaris means “hair.” KP is harmless, and it’s not infectious. Even though there’s been a lot of research looking into keratosis pilaris, we’re still not sure of its exact causes.
What we do know is that those bumps form when excess keratin — the main protein that makes up skin, hair and nails — builds up inside your hair follicles. It forms a little plug, and may or may not trap the hair inside. Sometimes patients get a bump here and there, or it can show up in patches, most often on the back of your arms.
KP tends to run in families, so we suspect there’s a genetic component there. It’s also associated with atopic dermatitis, or eczema, which means we often see the two together. This could be due in part to a genetic mutation that diminishes the effectiveness of our skin barrier. There’s also some evidence to suggest that a lack of sebaceous glands — responsible for producing oils in the skin — can cause problems within the hair follicle and lead to that buildup of keratin.
Dr. Pimple Popper's KP Picks
How can you tell the difference between KP, acne, and ingrown hairs?
DPP: I get this question all the time, because sometimes little bumps on the skin can look very similar to each other.
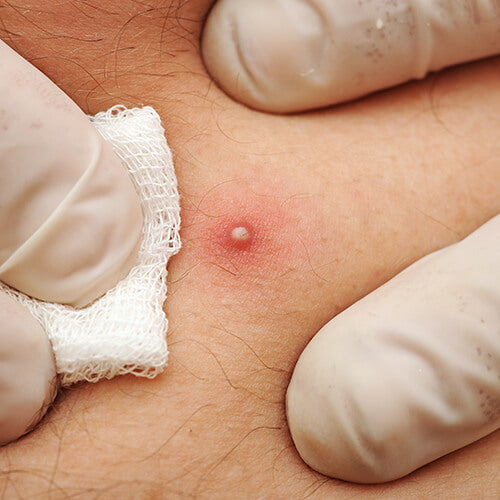
In terms of pimples, we sometimes see whiteheads on the body, but those tend to be a bit larger than KP bumps. Papules and pustules will be red, and possibly painful. In general with acne, we see it on the body in areas with a higher concentration of sebaceous glands, like the chest and shoulders.
Ingrown hairs can pop up anywhere, but if you see a bump in a commonly shaved area, chances are it’s an ingrown hair — especially if you notice some inflammation. Ingrown hairs, too, are often larger than keratosis pilaris bumps.
So the main things to look out for with KP are tiny, rough bumps that show up in areas where skin is dry. Sometimes when you scratch one of those bumps, you’ll notice that a little ball of white keratin will come off of your skin. It’s different from the contents of a pimple, because it’s harder and more solid. Don’t pick at your keratosis pilaris though, or you could cause an infection.
How do you treat keratosis pilaris?
DPP: While we don’t yet have a cure, the good news about KP is that we can manage it very well with topical skincare. Alpha hydroxy acids in particular work extremely well because they exfoliate and help soften up those keratin plugs. Two of my favorites are glycolic acid and lactic acid, which not only exfoliate but help stimulate the skin to produce more natural moisture.
I’m a fan of treating keratosis pilaris with a dual approach of regular exfoliation, plus moisturizing — that seems to produce the best results for my patients. That’s why I created my SLMD Body Smoothing System, which includes Glycolic Acid Body Scrub for the shower and Glycolic Acid Body Lotion to lock in the moisture while continuing to exfoliate.
Some patients tell me that their keratosis pilaris gets worse in the wintertime when their skin is drier, while others experience it year-round. I always recommend sticking to your skincare regimen to just keep your KP under control.